Worried fraternity says young doctors dying because of long work hours, no proper gear

A medic collects a swab sample of a girl at a health care centre
Dr Pratiksha Waldekar, 32, a pathologist, was seven months pregnant and was working at a private dedicated COVID hospital in Amravati. She contracted the virus and delivered a still born child. Her condition deteriorated and she died on September 20.
Dr Prashant Jagtap, 26, who worked at a private, non-COVID hospital in Amravati, contracted the virus a month ago and died on August 4, a day before his wife delivered a baby boy. He was the sole breadwinner.
ADVERTISEMENT
Dr Ketaki Paranjape, 33, an anaesthesiologist at a private medical college in Chiplun and alumnus of Grant Medical College, Nagpur, lost her battle against COVID-19 on September 15.
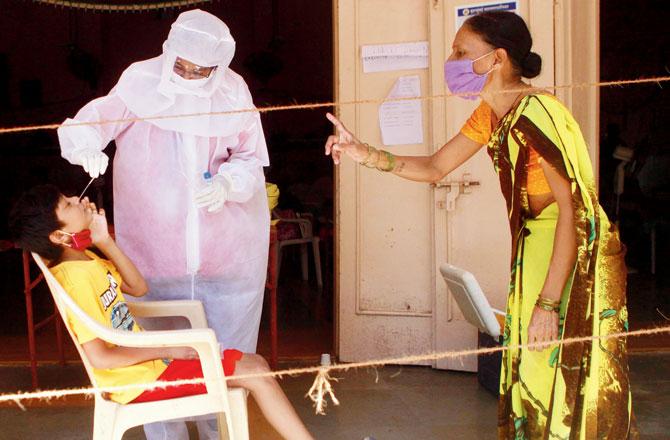
Civic medical staff collect samples for COVID-19 test, at Vanita Samaj, Shivaji Park, on Monday. Pic/Ashish Raje
They are among the 450-plus doctors who have lost their lives fighting COVID-19 till September 28 across the country, but what comes as shocking to doctors is that several of them were young experts, like anaesthetists, surgeons, paediatricians, gynaecologists, aged between 25 years and 45 years.
Dr Hriday Chauhan, a paediatrician from Azamgarh, Uttar Pradesh, told mid-day, "In the past couple of weeks, we have come across cases of young experts dying of COVID-19... We have compiled data of the frontline doctors who have died [during the pandemic] across the country, through our networks and media reports. As per our data, Maharashtra was initially reporting the most deaths of health care workers, but now, the number of deaths of young professionals is on the rise in Kerala, Karnataka, Tamil Nadu, and West Bengal."
"We have now realised that these young doctors are coming in direct contact with COVID-19 patients almost daily, which results in virus load. Moreover, in case of paediatricians, the infants may be carriers of the virus, through their asymptomatic parents." "Anaesthetist and surgeons are working with emergency patients and in the process of saving lives, they overlook their own safety," explained Dr Chauhan.

(From left) Dr Pratiksha Waldekar and Dr Prashant Jagqtab died of COVID-19 in Amravati, and Dr Ketkai Paranjape died in Nagpur
Dr Wiqar Shaikh, senior allergy and asthma specialist, said, "The entire medical fraternity worldwide is worried about morbidity and mortality of frontline healthcare workers, especially doctors."
An analysis by Amnesty International on September 22, 2020, revealed that over 7,000 healthcare workers, mostly doctors, worldwide have died of COVID-19. The causes for these deaths are: a) surge in COVID-19 cases and b) a dire shortage worldwide of protective gear, such as N95 masks, gowns, gloves and PPE kits.
In India until September 16, 382 doctors had died of COVID-19, as per reports from the Indian Medical Association, said Dr Shaikh. However, this figure is likely to be higher. In fact, the Centre for Disease Dynamics, Economics and Policy in Washington DC has said that India's system of recording death is weak and that the possibility is that many more healthcare workers have died in India so far.

Dr Asit Khanna, senior cardiologist from Ghaziabad, UP
The root cause of the problem is that India spends only 3.6 per cent of its GDP on healthcare, which leads to poor health infrastructures, shortage of doctors, health care workers, medical equipment and definite shortage as compared to other countries of protective equipment.
What is shocking in India is the death of several doctors in their 20's and 30's. It is estimated that doctors suffer four times the mortality of ordinary citizens, because they are constantly in contact to COVID-19 patients.
When asked about the reason behind young doctors dying of the disease, Dr Shaikh said the senior doctors may have decided to stay away, so the resident and young consultants are involved in day-to-day management of patients, including physical examination and procedures, in the ward and Critical Care units – like injecting, starting iv fluids, collecting blood samples, incubating bad patients for ventilators, carrying of cardio respiratory resuscitation in patients who are declared almost dead. The young doctors come in physical contact with COVID-19 patients and with no standardised PPE kits or face mask, their protection has become a serious concern.
"The frontline doctors are more vulnerable to the infection, and the Indian Medical Association have reported 382 doctors' deaths across the country so far. The initial profile of doctors' death analysed in a study in April 2020 showed 90 per cent were men, and 66 per cent were aged above 60 years, and 80 per cent had comorbidities. Thereafter, doctors who were in high risk profile were advised to stay away from active practice, and subsequently the profile shifted to deaths among young doctors who were likely to be males, in high-risk practice such as emergency care, anaesthetists, dentists, ENT specialists, general practitioners, internal medicine, surgeons, etc, in reducing order of frequency," said Dr Subhash Hira, professor at Global Health at the University of Washington-Seattle, US, and health adviser to several UN, Indian and African health agencies.
Also Read: 89 local body doctors quit, allege ill-treatment by officer in Maharashtra
Dr Hira added, "The India health workforce is 2.5 times more vulnerable to COVID-19-related deaths compared with the general population's COVID-19 death rate of 53/million population. The likely problems lie in the weaknesses in its health systems that include the following: physical distancing between infected patient and treating doctor is generally <1 foot due to professional needs [when ideal distancing for COVID-19 prevention is recommended to be > 6 feet), delayed provision of appropriate, well-fitting and adequate personal protective equipment (PPE)."
He continued, "The lack of containment of patient aerosol by use of polythene tent surrounding each bed and having negative pressure air circulation in these wards, low density of 9 lakh doctors i.e 692/million population leading to over-burdened doctors, poor sanitation in overcrowded healthcare facilities that were quickly erected across the nation, and slow community participation in preventive measures. The lack of scientific and operations research has made it difficult for policy implementers to improve performance and efficiency of systems, and improve work safety of doctors.".
Dr Ketan Vagholkar, professor of surgery at DY Patil Medical College, said, "Supportive care continues to be the mainstay of the treatment. Hence, individual immunity is the most important factor, which can prevent infection spread."
Dr Vagholkar added, "Adequate sleep, of at least seven hours, good nutrition fortified with vitamins and regular exercise, will help in maintaining strong immunity. Healthcare workers have to work for prolonged hours to treat the increasing number of patients. The standard work protocol, which was initially proposed for frontline healthcare workers, has been modified due to the increase in demand of the medical workforce. As a result, frontline health workers have to work for longer shifts with PPE kits. The interim rest period has been decreased and increased stress with irregular eating habits has led to compromise of their immunity. As a result, even younger healthcare workers are getting infected."
"However, as most of the patients are asymptomatic, they are advised home quarantine. This has significantly reduced the turnover of patients coming to OPD. Young healthcare workers have to take utmost care of themselves by meticulous use of PPE kits, adequate nutrition, good sleep and exercise whenever possible. They should avoid compromise in self-protection due to COVID-19 fatigue, which increases tiredness and stress. This has to be avoided at any cost," said Dr Vagholkar.
Act before it's too late
Dr Asit Khanna, a well-known senior cardiologist from Ghaziabad, UP, has started a Facebook page -- Corona Fatalities and Infections in healthcare workers Worldwide. He said, "Dr Shatrughan Panjwani, 62, is believed to be the first frontline warrior who died of COVID-19 in the first week of April, and since then the number is only going upwards."
"We must understand that we in a war against COVID, but unfortunately, unlike our armed forces, who are well trained and well equipped, to fight our enemies, the healthcare workers have been left in the lurch with no training or safety gears, and worst, no specialised equipment to fight the virus. We have no standardised PPE kits and safety gears, a couple of weeks ago, even though they were in short supply," said Dr Khanna.
"We are in a situation where the COVID-19 numbers are increasing with every passing day and we, the frontline warriors, have no reserved bed for when we contract COVID-19. I have come across numerous cases where frontline warriors had to be taken to three to four hospitals, and by the time a bed was arranged it would be too late," said Dr Khanna.
"Our frontline young warriors are getting affected due to virus load with every day exposure to the COVID-19 patients in ICU and wards, treating the sick and bad patients, our own foot soldiers have become sic now and the government has not only reduced the quarantine period, but have now almost brought it down to two days leave and some places due to staff shortage, it has become long working hours and if nothing," he concluded.
Keep scrolling to read more news
Catch up on all the latest Mumbai news, crime news, current affairs, and a complete guide from food to things to do and events across Mumbai. Also download the new mid-day Android and iOS apps to get latest updates.
Mid-Day is now on Telegram. Click here to join our channel (@middayinfomedialtd) and stay updated with the latest news
 Subscribe today by clicking the link and stay updated with the latest news!" Click here!
Subscribe today by clicking the link and stay updated with the latest news!" Click here!







