Special stem cell procedure, performed for the first time in country, makes toddler with complicated form of leukaemia and less that 10% chance of survival, completely cancer-free
At just three years, Aadiya Nair has had enough treatments and hospital visits to last a lifetime. But, the child, who has battled acute leukaemia and its associated complications since she turned two, is a happy, healthy toddler today, thanks to a first-of-its-kind haploidentical transplant (a stem cell procedure) performed in the country.
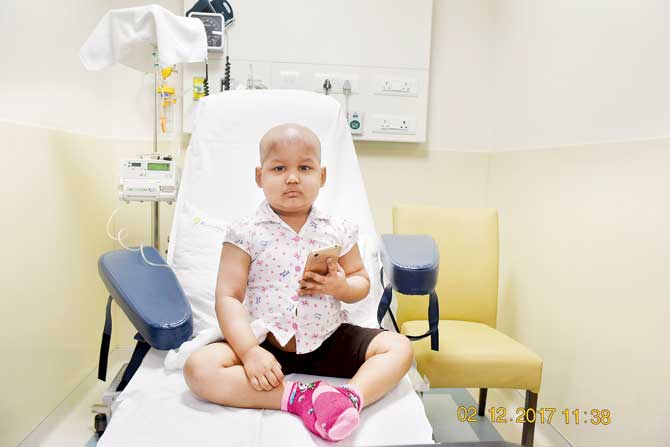
Aadiya Nair
Aadiya had tested positive for acute leukaemia (blood cancer) last year. She underwent five intensely gruelling cycles of chemotherapy and medication, but within a year, her devastated parents were told that she had relapsed (around 20% of children relapse). Moreover, because she had relapsed in the very first year of treatment, her case immediately became high-risk.
Dr Shweta Bansal, paediatric hemato-oncologist, said, "The only cure was a bone marrow transplant. Unfortunately, the child did not have any matched sibling or a related or unrelated donor for the transplant. So, we decided to counsel the parents about a haploidentical transplant, wherein the parents can be donors."
She added, "While haploidentical transplants have been performed in India for the past two-three years, they are mostly done through conventional methods, which have high chances of GVHD (graft disease) and mortality. In Aadiya's case, we performed the transplant using the latest technology by removing all unwanted cells (which cause GVHD) and also infusing useful cells (for rapid immune reconstitution to prevent post-transplant infections) from the donor stem cells."
"Another advantage of this procedure is that the cost fell to a fraction of what the child parents would otherwise have had to spend had they gone abroad. The approximate cost for such a treatment can run into more than a crore in a foreign country," Dr Bansal said.
The background
Recounting their first tryst with the dreaded C-word, Suresh Nair, Aadiya's father said, "We noticed bluish spots all over her body but thought it may be an allergy. We never imagined it could be something as terrible as cancer. The first few weeks were extremely difficult for us. Both of us [Suresh and Aadiya's mother, Shruthi] used to look at our child and start crying."
Suresh added, "At some point we decided to fight for our daughter's life." Through friends, Suresh took Aadiya to Dr Mahesh Balsekar, senior paediatrician at HN Reliance Foundation hospital. Dr Balsekar realised something was seriously wrong and referred the child to Dr Bansal.
Dr Bansal said, "Adiya responded well to the initial treatment of chemotherapy and other medications and her maintenance treatment was started in November 2016. It was during her second maintenance cycle that her platelet counts dropped. She underwent bone marrow examination again and our most dreaded fear came true, she had relapsed."
Dr Bansal added, "It was a difficult situation, as on-treatment relapses are high-risk, with not more that 20-30% chance of survival. The only way to improve survival rate in such cases is bone marrow transplant. However, Aadya did not have any siblings. Matched sibling donors are the best for such transplants."
No donor in world registry
Dr Bansal said, "We sought the advice of national and international experts. A variety of treatments was suggested, including newer drugs such as blinatumumab and CART Cell. These are all very expensive. We did a worldwide search for unrelated donors but unfortunately couldn't find a match for Aadiya," the doctor said.
The only way to go was haploidentical transplant. While Aadiya and her parents were being prepared for it, the child developed another dreaded complication, HLH (haemophagocytic lymphohistiocytosis), a life-threatening immunodeficiency, and secondary dengue, which not only delayed her treatment but also required heavy doses of steroids and other immunosuppressive drugs to bring her condition under control. With this new complication, the situation was becoming difficult. In conventional haploidentical transplants, where post-transplant cyclophosphamide is given, there were chances of HLH getting reactivated.
New haploidentical transplant
Dr Bansal said, "The only option was to try the new haploidentical procedure. This kind of an advanced procedure has been done for the first time in India. We had to go for a technology that causes removal of naïve T cells (which cause GVHD) and infuse memory T cells (which help in recovery of immune function) with heavy doses of stem cells. Her father was finally selected as a donor, and he got a few injections to increase the number of stem cells in his blood. We got a yield of cells, which we then infused. Miraculously, Aadiya's counts recovered in nine days post transplant. She did very well."
Dr Bansal said the hospital was able to perform the procedure for one fourth of the cost. Suresh, who work with a logistics company in Pune, is the sole breadwinner earning a monthly salary of R25,000. He said, "Apart from mortgaging Shruti's jewellery, we had to take financial assistance from friends and relatives. One of our relatives mortgaged his property to raise funds for Aadiya's treatment. Also a few charitable trusts and Reliance Foundation pitched in to support us."
 Dr Shweta Bansal with the Nairs and Aadiya
Dr Shweta Bansal with the Nairs and Aadiya
Transplant, a success
Aadiya underwent the procedure in September and more than 60 days have passed, with her showing no complications. Proper care needs to be taken for at least the next few weeks.
"She will be like a normal child and can go to a regular school, we are positive that she will never have a relapse of the ailment in future and can lead a normal life," Dr Bansal said.
"For us, Dr Shweta was a godsend. She never gave up hope of Aadiya's recovery and stood beside us throughout. Sometimes, miracles do happen," Suresh said. The treating doctors will soon be getting their details sent for publishing in international medical journals with Aadiya's case study.
Catch up on all the latest Mumbai news, current affairs from Mumbai, local news, crime news and breaking headlines here
Download the new mid-day Android and iOS apps to get updates on all the latest and trending stories on the go
 Subscribe today by clicking the link and stay updated with the latest news!" Click here!
Subscribe today by clicking the link and stay updated with the latest news!" Click here!







