India’s Medical Termination of Pregnancy Act predates the law in America. Yet, Indian women, who know they have the right to a legal abortion minus guardian, take risk to dodge shame

Mumbai-based advocate Shivani Shah says a friend who chose a Ghatkopar clinic over a Bandra hospital for an abortion has found it hard to conceive after too much scraping left her uterus lining flimsy. Pic/Ashish Raje
After bleeding most of the night on the pot, Anushree Majumdar lay down on the floor to catch a few winks before the morning turned. “I was bleeding what felt like litres of blood,” says the 38-year-old, “and the floor would be easier to clean up. I had to wait until 9 am, when the gynaec down the road from my apartment would open.”
Majumdar, then 24 and a journalist in Delhi, was three months pregnant, but didn’t know it. “I was glad to have just broken up with a toxic boyfriend,” she says. “This was in 2008, when social media was not the landscape of our life, and medical conditions such as PCOS [Polycystic Ovary Syndrome] were not on our radar. I wasn’t tracking my periods and had never been pregnant before, so I missed all the signals my body was sending. My period was erratic anyway, sometimes 40 days apart. I worked odd hours, ate out a lot and was overweight, so becoming a little more rounded was not unexpected. I didn’t have morning sickness, but in hindsight, I realise that the overpowering desire for chocolate was a strong indicator. I was a slave to that craving.”
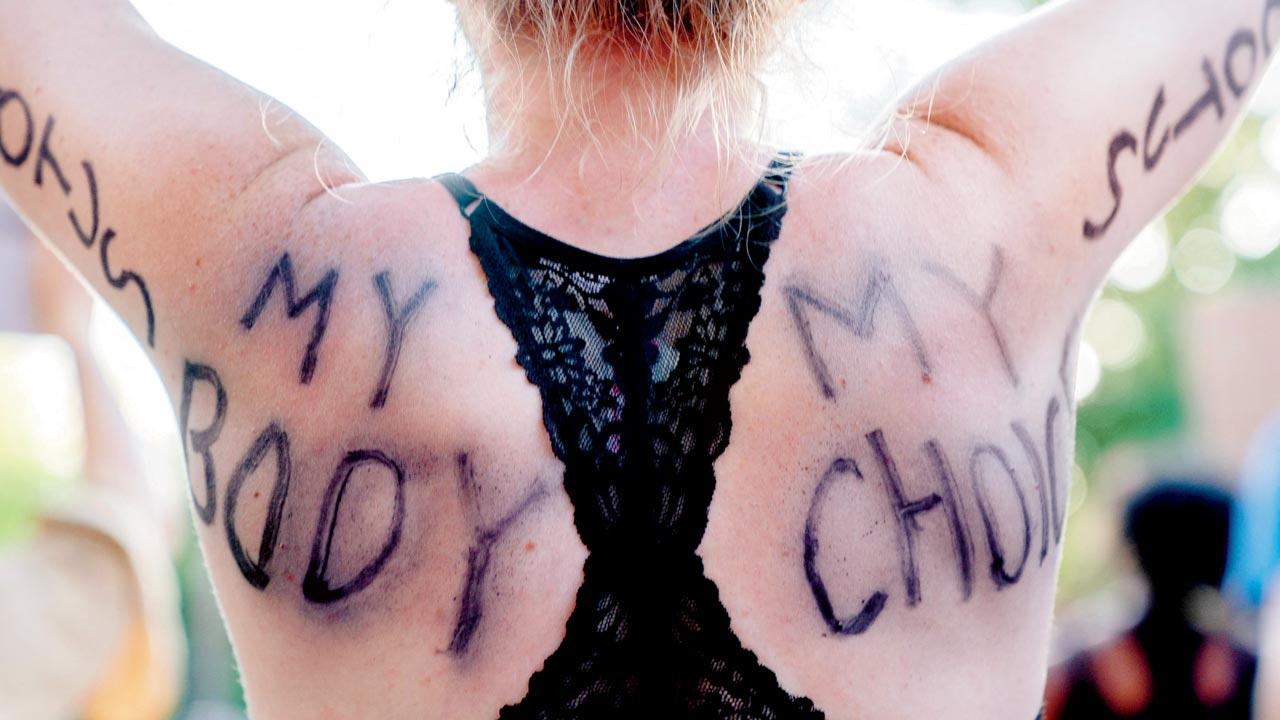 Abortion rights demonstrators in Maryland, US, last week. The US Supreme Court on June 24, 2022, ended the right to abortion. Pic/Getty Images
Abortion rights demonstrators in Maryland, US, last week. The US Supreme Court on June 24, 2022, ended the right to abortion. Pic/Getty Images
Cutting short a late-night assignment, she had rushed home because she was bleeding heavily, and was in excruciating pain. “I wanted to get home while I still had the strength to climb up three flights of stairs to my apartment. I was using sanitary pad after pad and the discharge was thick, and clumpy,” she says. As she sat on the toilet, flushing away the blood, she realised this wasn’t menstruation; she was haemorrhaging. Her body had miscarried and was now expelling the foetal growth.
She rose from her “world of pain” and made her way to the government hospital down the road. There, the judgment began. “The gynaec was dismissive and matter-of-fact,” remembers Majumdar, who is now an independent editor in Mumbai. ‘Tumhe pata nahin chala tum pregnant ho? Akal nahin hai?’ she scolded me. The physical examination was also rough. She slapped on a pair of gloves and probed deep without warning me. She told me I was probably pregnant, but couldn’t be sure without an ultrasound. She said I would continue bleeding today and should take the day off. I told her I didn’t have the time!”
 Apoorva Mohan
Apoorva Mohan
“Tumhe rest karna chahiye, but you think you are Super Woman,” the doctor scolded her again.
Majumdar had just exited a relationship with a fellow journalist; he offered money for the abortion when she informed him of her miscarriage. Her family was in Kolkata and she was working long shifts at her daily newspaper. She tried to call in sick but there wasn’t a colleague available to replace her at such a short notice.
 Women shout slogans against the Irish government for the death of Savita Halappanavar, who died in Ireland after doctors allegedly refused her an abortion in 2012. Pic/Raveendran/AFP via Getty Images
Women shout slogans against the Irish government for the death of Savita Halappanavar, who died in Ireland after doctors allegedly refused her an abortion in 2012. Pic/Raveendran/AFP via Getty Images
The gynaecologist wrote down a prescription for an injection that would stop the bleeding and help with the pain. “The hospital was so shabbily run that their own pharmacy was not functional and I had to go to the chemist across the road. He of course, knew what the injection was for, and radiated judgment,” she says. At work, she told her boss she had a medical appointment at 5 pm (which is the middle of a work day for journalists) that she couldn’t miss. “Everyone at work could see I was in pain, but my boss was pissed and wasn’t sure I would return, so he asked me to use her car and driver.”
Majumdar was the first patient at the gynaec in the morning, but in the evening at the diagnostic centre, she was among women in varying stages of pregnancy. With so many patients, the procedure had the efficiency of a factory line. “The doctor there told me I had been pregnant, and then my gynaec loudly declared, ‘Haan Haan, missed [carriage] hai, missed hai.’” Majumdar still needed a MTP (Medical Termination of Pregnancy) to expel what was left lest it turn septic.
 Shivani Shah
Shivani Shah
Then there was the question of money. “I was making R24,000 a month, and on that day I had Rs 600 to my name,” says Majumdar. “I needed to pay for the consultation, buy medicines, do the ultrasound, then the procedure and post-op medicines. I knew I couldn’t talk about this to anyone. I was close to two editors at work, and one of them immediately took over the situation and helped me. Meanwhile, I called my parents and told my mother to wire me some money for an emergency ‘clot-removal’ surgery. My mother, who probably also has no experience of an abortion, thought I had inherited her propensity to ovarian cysts.”
On Monday, Majumdar wore her best party dress to go to the hospital. Her colleague accompanied her and signed the required paperwork and paid. While preparing for the surgery, the nurse implementing the pre-op procedure added to the institutional moral policing. “Condom use nahin kiya? Pregnant kaise ho gaye?” the nurse asked. “They are desensitised,” says Majumdar. “You know that within an hour, you are going to be faceless and nameless.”
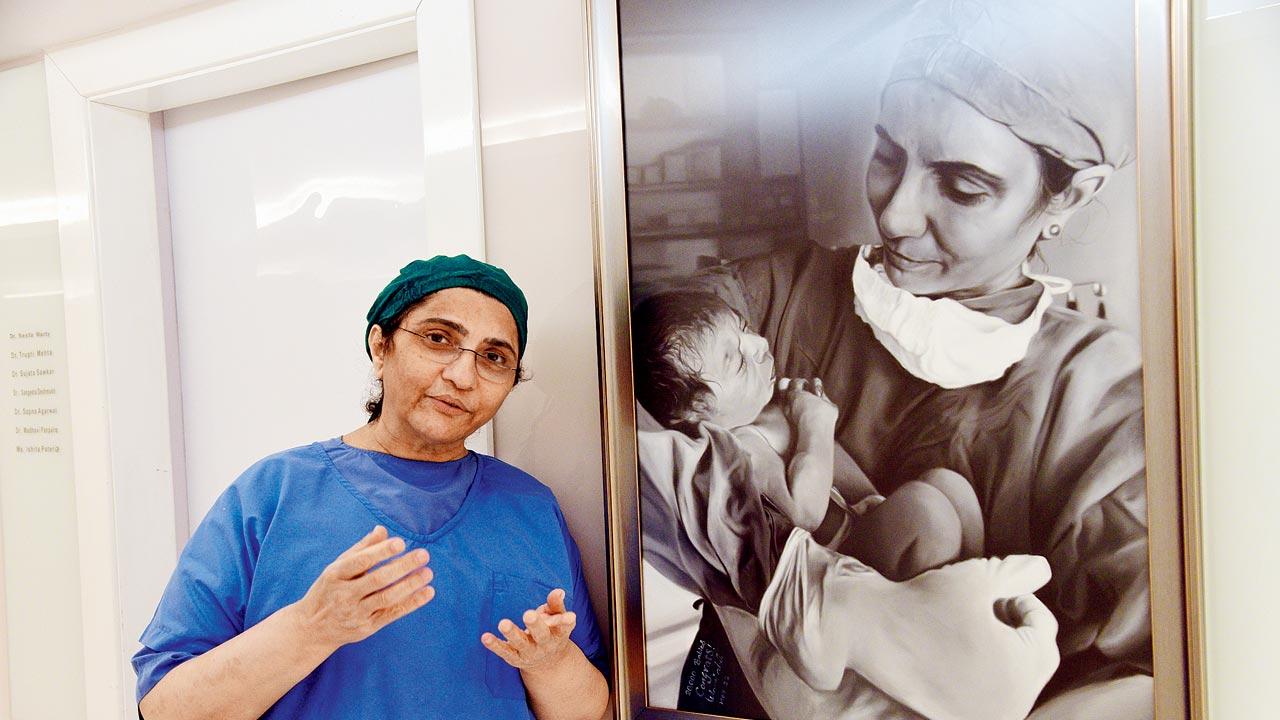 Dr Firuza Parikh, Director of the Jaslok FertilTree International Fertility Centre, believes that it’s important that a doctor understands the circumstances of the patient, be non-judgmental and guide the patient through a difficult emotional phase and also protect their physical health. Pic/Pradeep Dhivar
Dr Firuza Parikh, Director of the Jaslok FertilTree International Fertility Centre, believes that it’s important that a doctor understands the circumstances of the patient, be non-judgmental and guide the patient through a difficult emotional phase and also protect their physical health. Pic/Pradeep Dhivar
Mazumdar’s pregnancy was the result of a toxic boyfriend’s refusal to wear a condom. But that is not the point.
As the MTP Act, 1971 stipulates, women in India have the right to a medical termination of pregnancy by a registered medical practitioner, without the permission or without being accompanied by a guardian if she is over 18 years of age and is not mentally challenged. The pregnancy should not exceed 12 weeks, and in the case of termination between 12 to 24 weeks, at least two registered medical practitioners must be of the opinion that there is risk to the life of the woman or of grave injury to her physical or mental health; or substantial risk that if the child were born, s/he would be seriously handicapped.
 A file photo of Niketa Mehta and her stockbroker husband Haresh leaving court. In 2008, the Bombay High Court rejected a plea by the couple from Bhayandar seeking to abort their 25-week unborn child who was found to have congenital heart defects. It was a case that generated furious debate over the ethical implications of the law on abortion. The court rejected their plea after the two medical reports presented opposite views. The case had opposed a direct challenge to certain sections of the MTP Act since Niketa’s pregnancy was well beyond the legal limit for abortion. Pic/Getty Images
A file photo of Niketa Mehta and her stockbroker husband Haresh leaving court. In 2008, the Bombay High Court rejected a plea by the couple from Bhayandar seeking to abort their 25-week unborn child who was found to have congenital heart defects. It was a case that generated furious debate over the ethical implications of the law on abortion. The court rejected their plea after the two medical reports presented opposite views. The case had opposed a direct challenge to certain sections of the MTP Act since Niketa’s pregnancy was well beyond the legal limit for abortion. Pic/Getty Images
“The Roe v Wade decision [the 1973 landmark decision in which the US Supreme Court ruled that the Constitution of the United States generally protects a pregnant woman’s liberty to choose to have an abortion] came two years, in 1973, after the Indian MTP law was enacted,” says Advocate Shivani Shah from Kay Legal and Associates, “So in that sense, we were ahead of them. Because of our population control measures, most women, even in the villages, are aware that they have a right to abortion and can go to any government hospital. It’s the actual act of going, because of the moral policing, that is the impediment. They prefer to go to a smaller backyard or garage clinic to avoid shaming. This is why the official rate of abortion in India is not high.
While technically, an MTP may be performed if the health of the woman or the child is at risk, the municipal form that one needs to fill up for the procedure is far more understanding. “Among the reasons listed for the MTP is ‘Failure of contraceptive’,” explains Shah, “It’s discreet and doesn’t need explanation or evidence. It’s the most
ticked option.”
The “efficiency” of garage clinics lays a lot less emphasis on post-op care, hygiene, and sterilisation of implements is questionable. “My friend got pregnant a few years ago and chose to go to a small clinic in Ghatkopar, instead of a hospital in Bandra where she lived, to protect her identity,” says Shah. “They scrape the lining of the uterus during the procedure, and in her case—probably because they were doing four to five terminations in a day—they scraped more of the lining. It made the uterus very thin, and as a side-effect it’s hard for the foetus to latch on now. This has affected her chances of having children now—it’s 70 per cent with effort, as opposed to 100 per cent. She has already had two miscarriages.”
Dr Shiraz Vazifdar, a gynaecologist and obstetrician at PD Hinduja Hospital emphasises that the MTP Act empowers women and it’s important to go to a recognised, well-equipped, certified MTP centre and qualified gynaecologist to ensure the future reproductive health of the woman.
However, as noble as that is on paper, more than one woman has been denied quality care by a doctor. Meera (name changed) was 23 when pregnant, and flew down from the Gulf to India to terminate her pregnancy. She cautiously chose to a city that was not her hometown and opted for the best medical attention dirhams could buy in a luxurious hospital. “Come with your mother,” the gynaecologist told her, turning to the nurse to say, “they all have sex and fun, and then come to us. I won’t do it without your parent’s consent.”
Legally, you don’t need to be accompanied by anyone if you are over 18 years of age. Hospitals insist that the woman brings someone along to help the patient go home and avoid liability later; say, an angry husband who was unaware and arrives to pick a fight with the doctors later. An adult woman does not need the permission of a husband or family to get a hysterectomy either.
Dr Firuza Parikh, Director of the Jaslok FertilTree International Fertility Centre, does not undertake MTPs due to personal beliefs. But says, “The reasons for MTP may vary and have different circumstances. Empathy goes beyond bedside manners. A doctor has to understand the circumstances of the patient, be non-judgmental and guide the patient through a difficult emotional phase and also protect her physical health. It is the patient’s prerogative to be treated with respect and not be humiliated. A physician who does not wish to perform an MTP can always refer the patient to someone who does.”
Morally and constitutionally, this would extend to all medical staff. At 22, this writer found herself undergoing an MTP in a small, homely clinic. As she got emotional under the effect of the anaesthesia, the anaesthesiologist asked her: “Then why did you have sex.”
It’s this dehumanising attitude, says Apoorva Mohan that prompted her to collate a list of sex-positive gynaecologists. The 30-year-old, who works in a creative design studio, started first with her hometown of Chennai, and was soon creating a list for Bangalore and Kochi. Hyderabad is next. “Resources are even harder to come by in Tier 2 and Tier 3 cities,” she says. She asks for personal references on social media, checks the doctor’s rating on Google and holds out for at least two verifications per doc.
Her project was also sparked by experiences her friends had. “In 2014-15, a close friend got pregnant,” she says, “She was 24 years old and we tried looking for a good gynaec. Social media was not yet as resourceful as it is now. We went to the doctor with the highest rating and while she was impersonal, the staff was disapproving. ‘Isn’t it bad you are having sex without marriage,’ a nurse asked when the doctor was out of the room. When we told the doctor, she did not reprimand the nurse, nor did she assuage us. They also asked for unnecessary details, such as her father’s name and occupation. Her partner accompanied her but was made to sign the release form as husband, though they both protested. The doctor shrugged this off as standard procedure.”
Another pregnant friend, says Mohan, had family support, which made all the difference. “Her mother was understanding. She put a mangalsutra around her daughter’s neck, and told the doctor she was married.”
If the country would admit that its people have sex outside marriage, professional medical care could become right. Whether the system does or does not catch up, a salve can come from other places.
Majumdar says, the trauma is not as much the MTP as it is having to go through the process alone in a climate of shame. Many years later, she told her mother that she had had an abortion. “She was silent for a few heartbeats and then I could hear her sobbing softly on the other end of the phone,” she says. “When she spoke, the first thing she said was, ‘I am so sorry you had to go through this alone.’ It was a balm I didn’t know I needed. I may not have gotten care from the system, but my mother’s response as a woman and a mother soothed me. When she came to visit me in Delhi, she met my colleague to thank her for being with me right through.”
12
No. of weeks the pregnancy should not exceed for an Indian woman over 18 years and of sound mind to get an abortion by a registered doctor
Controversial US abortion ruling

On June 24, the US Supreme Court ruled in favour of a strict Mississippi abortion law, thereby overturning the Roe v. Wade landmark ruling that established the constitutional right to abortion for almost 50 years. Women rights activists feared that this would lead to all but total bans on the procedure in about half of the states in America, and said this infringed on the right of women on their own bodies.
 Subscribe today by clicking the link and stay updated with the latest news!" Click here!
Subscribe today by clicking the link and stay updated with the latest news!" Click here!






